My Experience With The Gupta Retraining Program for Chronic Fatigue Syndrome

As many of my readers know, I struggled with chronic fatigue syndrome for almost seven years and wasted a small fortune on supplements and therapies that did not help. The Gupta Program certainly was not one of them.
In this article, I will be sharing my personal experience with the Gupta Program, exploring the theory behind it, and explaining when it may or may not be an appropriate tool for those struggling with chronic fatigue syndrome.
Origins of the Gupta Retraining Program

Ashok Gupta was studying economics at Cambridge when he developed chronic fatigue syndrome. ‘Burning the candle at both ends’ he began experiencing a flu-like illness. After recovering from the acute phase he developed unremitting fatigue, unrefreshing sleep and an inability to focus.
After repeating the year, he ‘scraped’ through his studies, and for many years after the following symptoms persisted:
- Unremitting Fatigue
- Joint and muscle aches and pains
- Unrefreshing sleep
- Depression and Anxiety type symptoms
- Headaches
- Emotional Lability
- IBS symptoms such as Bloating and Constipation
- Food Intolerances and sensitivities
After conducting his own research, he believed that the development of CFS in a large subset of patients arises from a chronic ‘hyperarousal’ and ‘re-conditioning’ of the brain’s limbic system.
In other words, during the onset of CFS, people tend to be very stressed for prolonged periods of time. This conditions the brain to ‘overmonitor’ the physical symptoms. Consequently, the brain gets ‘locked in’ to a state of ‘subconscious’ hypervigilance to symptoms helping drive an exaggerated ‘stress’ response and maintain the symptoms of CFS.
If it’s not clear, don’t worry. I’m going to explain it in more detail later.
After formulating his idea, Ashok retrained to become a (Neuro-Linguistic-Programming) coach and set up a clinic on Harley Street, London, helping people with CFS, Fibromyalgia and other chronic conditions. Over time he observed some very similar patterns during the onset of the condition.
Most of his clients were going through an extremely stressful time in their lives, and typically felt unable to cope and developed a flu-like illness. After recovering from the acute phase they developed the symptoms of CFS.
Over time, Ashok crafted and honed several techniques into what is now the Gupta Retraining Programme or what was known as the Gupta Amygdala Retraining Programme.
Full disclosure: this is an extremely complex topic drawing on concepts and research from cognitive neuroscience, neuropsychology, immunology and endocrinology. At this stage, there are still more questions than answers, but the good news is, we do now have a better understanding of the concepts Ashok describes.
For the purpose of this article, I’m going to keep it ‘top-level’ but stay tuned for my upcoming series on neuroimmune conditioning and amygdala retraining where I’ll be taking a deep dive into the research exploring the possible role of neuroimmune conditioning in CFS.
The theory behind The Gupta Retraining Programme
Before we begin I think it’s important to cover some basics.
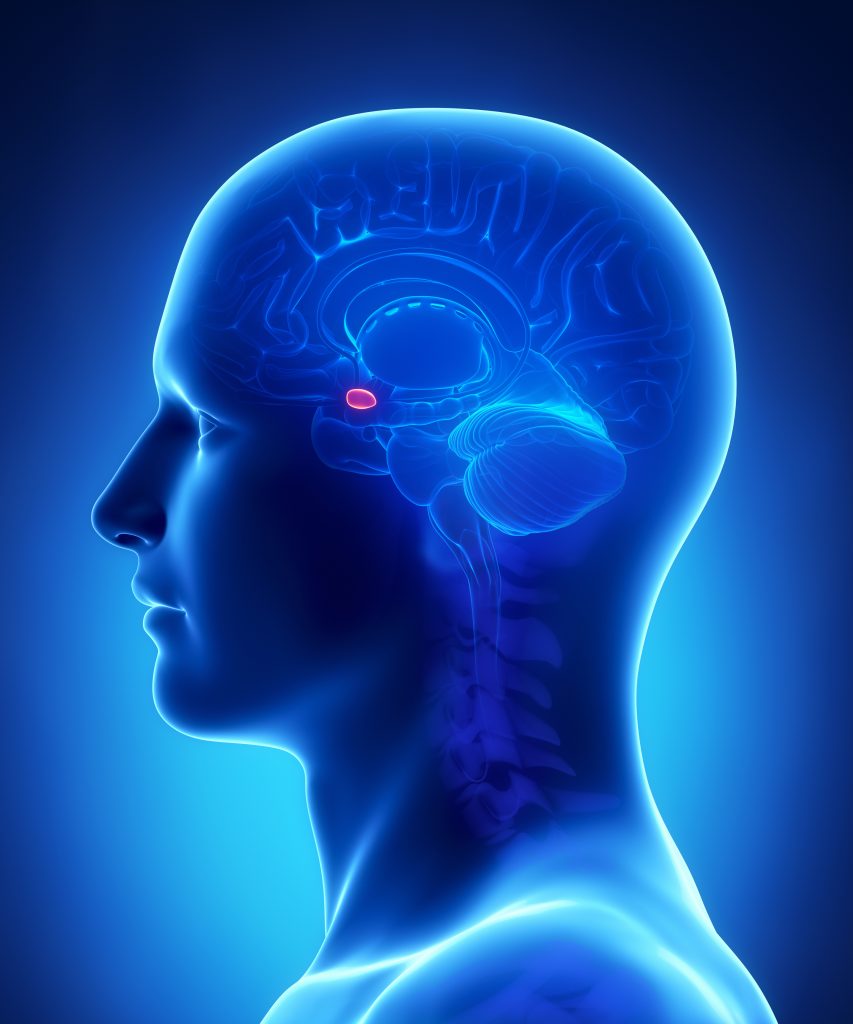
What is the Limbic System?
The limbic system sits just above the brain stem underneath the cortex and allows us to generate emotions, which are often subconscious and automatic. It comprises the amygdalae, hippocampus, thalamus, hypothalamus and cingulate gyrus. These structures are all working together.
What is the Amygdala?
The amygdala is often referred to as a singular structure but there are in fact two amygdalae which are almond shaped structures sitting on both sides of the brain.
They are our threat-interpretation and response system and modulate our memories of real or perceived threats.
In other words, the amygdalae recognizes a threat and helps us survive (e.g. moving out the way of a car). The amygdalae and hippocampus then work together to remember that event to protect you in the future.
The amygdalae are also central to our impulsivity and reward circuits. It plays an essential role in our incessant need for instant gratification. Issues affecting the amygdalae may be linked to issues such as depression, PTSD, phobias, anxiety and impulsivity.
Most importantly in CFS, the amygdalae help us monitor feelings we experience from our body and decide what’s important and what we need to pay attention to.
The prefrontal cortex
We now know there are many other structures involved in regulating and interpreting threatening information and this includes the prefrontal cortex, the insula, and the anterior and posterior cingulates.
The prefrontal cortex helps regulate and attempts to control impulses from the limbic system by finding the best possible response to incoming information. The connection between PFC and Amygdalae affects our ability to regulate impulsivity and emotion.
In other words, the prefrontal cortex is like the big brother: keeping things in perspective and telling us everything’s ok to protect us from being fearful, irrational, impulsive and emotional.
“Without the supervision of the prefrontal cortex, there’s no adult in the room. The emotionally immature child can run amok, lacking rules, discipline and boundaries”
David Perlmuter
The beginning of Chronic Fatigue Syndrome
Ashok believes that whilst anyone can develop CFS, people who tend to develop CFS are naturally more prone to stress and anxiety. This may be related to the modulation and attenuation of the immune system and its effect on our nervous and endocrine systems, but it remains unclear.
Ashok and the research suggests genetics, certain personality traits, poor sleep, poor diet and persistent and extreme stress (HPA-axis hyper function) may all play a role.
In practice, a common example is a person who is extremely driven and emotionally sensitive with a tendency to push beyond their physical limits to achieve a result. In the buildup to CFS, they won’t be sleeping or eating well (plenty of caffeine and sugar).
As Mel Collins beautifully describes in ‘the handbook for highly sensitive people’ these people tend to be ‘The Achievers’ ‘The Pleasers’ or ‘The Marytrs’.
During a time of great stress, patients begin to feel physically unwell often with a flu-like illness which develops into CFS.
It’s important to note, that although a viral flu-like illness is common, triggers can include pesticides, heavy metals, toxins, bacteria, parasites. In fact, Ashok argues any physical or chemical stressor on the body which occurs while the mind is experiencing acute psychological stress, can trigger CFS.
‘Priming’ or Hyperarousal of the Amygdalae
Warning: This part is quite lengthy so feel free to scroll down to the summary.
Ashok hypothesized that CFS begins when the amygdalae become highly aroused or ‘primed’ possibly due to environmental and biochemical factors. During a state of heightened arousal (emotionally traumatic time), when stress hormones are heightened, the amygdalae may become prone to learning “new sensitivities” or new things to be scared of.
Consequently, as acute symptoms develop, the limbic structures become conditioned to be highly sensitive to negative somatic signals or symptoms arising from the body. In other words, symptoms may be interpreted as more dangerous than they really are.
Eventually, ‘networks’ or cell assemblies are setup, which begin to create a disproportionate stress response relative to the threat the symptoms pose.
Additionally, as inflammation may have been present due to a virus or other pathogen during the fear conditioning period, immune activation may be re-triggered as memories of the conditions are recalled, helping drive inflammation.
Here is an example of an automated internal dialogue that maybe going on in a CFS patient:
Conscious internal dialogue: ‘ I’ve woken up feeling achy, Oh my gosh! There must be something really wrong, I can’t go to work!’.
Subconscious dialogue: ‘Oh no! I was achey when I developed this illness, this must mean I am still unwell, I must release stress hormones and activate the immune system to survive this threat’.
You maybe thinking, ‘but you said the prefrontal cortex plays a role in keeping things in perspective?’ In theory, yes, but as lab studies are demonstrating, chronic stress can cause ‘hyperexcitability’ of the amygdala and Ashok proposes that the ‘higher functioning’ structures such as the PFC can be ‘hijacked’ and help drive continuous attentional processes.
In other words, the PFC stops doing its job properly and makes it worse by diverting attention to health threatening information. Interestingly, researchers are finding people with CFS display attentional and interpretation biases to health threatening information versus healthy people who don’t.
(This may partly explain why conventional CBT have found reductions in fatigue as it is ‘interrupting’ the way patients interpret and attend to bodily feelings and symptoms.)
We are all aware of this process, whenever you’ve experienced an injury. Imagine, somebody walks up to you and cuts your arm and they run off. It begins bleeding. Your attention will immediately be drawn to the wound. You end up in hospital requiring stitches, meanwhile your mind is imagining all the consequences of this event. ‘What if I bleed out?’ ‘What if it gets infected?’ ‘What if I can’t go to work for a few weeks?’ ‘What if it happens again?’
Our attention will naturally be drawn to the present threat but in ‘healthy’ individuals (once the threat is over) the higher functioning parts of their brain will rationalise their thoughts, and allow them to get on with life with minimal interference.
But why do some go on to develop anxiety, depression, PTSD or chronic issue while others blissfuly just move on with their lives? We’ve all been ill, we’ve all had the flu at some point, why don’t we develop CFS?
We’re a long way from answering this, but I would be remiss not mention the work of Dr Ronald Ruden, a medical doctor and creator of the havening technique, used to reduce emotional traumas including PTSD, Phobias, Anxiety and many others. In 2015, a single session was found to reduce the symptoms of PTSD in soldiers returning from the Iraq war at King’s College London.
In one of his seminal papers, Dr Ruden describes four ‘requirements’ for a trauma or severe threat to be encoded into the limbic system:
- An event must occur (either first, second or third hand) (Having a horrible boss).
- Have meaning or ‘negative representation’ that is, be perceived as a threat and generate an emotional response (taking it personally).
- A vulnerable landscape: the electro-chemical state of the brain must be conducive at the time of the event. Dr Ruden believes an increase in number and permanence of AMPA (glutamate) receptors on the amygdala is required for traumatic encoding (heightened stress, poor sleep and poor diet).
- Perceived inescapability of the situation (bills to pay).
To Summarise
Coming back to Ashok’s theory, he believes that for some reason the inhibitory mechanisms of the prefrontal cortex and structures above become impaired and the limbic system becomes hyperexcitable and dominant driving grave fear and increased interoceptive attention on our symtpoms and feelings.
Ashok believes the amygdala ‘arrests’ the cortex because of the negative salience of the symptoms and the hippocampus brings back emotionally charged memories.
What all this jargon is saying (and if you remember anything from this article) is that in CFS our threat monitoring and response systems becomes ‘out of whack’ and at a subconscious level we become ‘fixated’ on the CFS symptoms which further drives symptoms through our stress response.
Ashok’s Medical Paper
In 2002, Ashok published a paper in the Journal Medical Hypotheses in conjunction with the University of Cambridge, where he discusses his theory. He went on to publish a research pilot in the ‘Journal of Holistic Healthcare’ in 2010 and most recently a study examining the effects of his programme on fibromyalgia in the Journal of Clinical Medicine.
How Ashok’s programme may work
I should add that this programme is not cognitive behavioural therapy (CBT) as you might have experienced in the NHS or your healthcare system.
Please not: There are one or two other programmes out including the dynamic neural retraining system by Annie Hopper and Dan Neuffer’s ANS Rewire Program, which are predicated on similar theories. I only have experience with clients using the Gupta Retraining Programme. Feel free to check out a review of the ANS Rewire Program by Graham from CFS-survivors blog.
The aim of the Gupta programme is to interrupt and retrain the signals from the amygdala, reducing reactivity of the nervous and immune systems whilst strengthening the inhibitory areas such as the prefrontal cortex (others include orbital cortex, insula and anterior and posterior cingulate).
In other words, to break the negative interpretations of signals coming from the body and helping the PFC (big brother) take charge and tell the limbic system (little brother) that everything’s ok.
In addition, the programme includes mindfulness training which in CFS patients has been shown to reduce amygdala reactivity and build grey matter volume in the prefrontal cortex and insula (a sign that new connections are being made).
My Experience with the Gupta Programme
I was extremely sceptical, as I really believed my CFS was caused by solely biochemical factors (virus, heavy metals and inflammation). Looking back, I don’t think I wanted to believe it could be caused by something else.
I didn’t want to believe ‘I conditioned myself into this’. Looking back, I believe I manifested CFS as a form of self-protection from a threatening world (which I mention in a previous article).
This does fit with the idea of amygdalae/limbic reconditioning, as the limbic system’s job is to make us feel fear and protect us from danger. This may be one of the reasons CBT can be effective, as it highlights our cognitive processes (aka general cognitive representation).
Within 2-3 weeks I noticed vast improvements in my energy and ability to work fairly normally without being exhausted the next day. The nice problem I had, was I would feel so good so quickly that I forgot to finish the programme. I would stop using the techniques and eventually the symptoms crept back.
I found myself stuck in this cycle for a few months until I realised the last few steps are crucial as it teaches you how to integrate back into normal life (which may actually be the hardest part for CFS patients i.e. believing we can return to normal life).
The programme does require persistence and discipline but having worked with many clients, they seem to improve fairly quickly.
Note: I used version 3 which came as a DVD box set. I understand Ashok has updated the programme to version 4 which is online. I believe the core techniques are the same.
What You Should Know Before Starting The Gupta Programme
At this point in time I remain unsure whether the Gupta programme can be used exclusively to reverse the symptoms of CFS. I certainly do believe it has the ability to improve symptoms by reducing stress and anxiety surrounding the condition, therefore, facilitating healing.
I therefore believe the biochemical elements of the condition need to be supported first with a relevant health professional.
Once the biochemical barriers are removed, the Gupta Program can repair the neurological legacy of the condition.
What came first? The Amygdala or The Immune System?
As with many chronic conditions, I believe there are multiple factors at play and what I strive to discover in the future is if the idea of amygalae priming is a result of neuroimmune factors or psychological factors resulting in neuroimmune effects?
To Summarise

If you are struggling with CFS and have been working with a professional to work through the biochemical issues and you still don’t feel you are making progress, I would highly recommend using the programme. If you are newly diagnosed or have not worked with a professional such as a nutritional therapist or functional medicine practitioner, I would start with addressing the basics first.
All I can say is both as a patient and practitioner having helped many people with CFS, I am extremely grateful to Ashok and his team for all they have done and I hope one day you may feel the same.
Wishing you well on your path to health,
Inder



11 Comments
Dalia kenig · March 9, 2021 at 3:58 am
Hi, I read on your website that you used applied kinesiology approach in your recovery. Have u used it to determine which supplements and dosages to take?
I have cfs over a yr now. I found blood tests and other test to be an endless chance and turned to nutritional response testing that used AK.
I am 4 months into this treatment. My baseline is 30% better and my energy is up and down
What was your experience like while doing the protocols?
Thxs
Inder Singh Virdi BA (Hons) mBANT · August 11, 2021 at 2:25 pm
Hi Dalia, my apologies for the delay. I did not see this. That’s excellent to hear you are seeing improvement. I must admit for the first two years it was a very difficult process with fluctuations in my symptoms. I found when I started protocols I would feel well and within a few days feel worse. I worked very closely with my practitioner and he was able to stabilise me. But it requires a lot perseverance, patients and positivity. Wishing you well. Inder
Daniel Kerlinsky MD · May 3, 2021 at 5:24 am
Thank you, Inder, for your report. In my osteopathic child psychiatry work I find the hippocampus swells from excess cortisol, becomes inflamed and then shrinks. The longer this process goes on… the further back the temporal lobe flattening becomes, especially on the left side. Eventually one loses the ability to maintain the story of one’s life.
Amygdala activation constitutes a totally different register of the emotional keyboard. Emotions that are so intense that we have found little can stop:
laughing so hard you can’t get up off the floor
crying so hard you can’t catch your breath
being so afraid you can’t stop shaking
not being able to get suicidal thoughts and urges to go away.
Amygdala heat is intense. Usually centered near the top of the ear it expands to on to even five inches in diameter in some people who seem to have a genetic propensity. It can slow venous drainage.
Demyelination is the most profound disruption of thought and emotional self-regulation. It can be triggered by relatively small stressors – like feelings of isolation or defeat. Demyelination of the uncinate fasciculus – a small bridge between the posterior frontal lobe and and the anterior temporal lobe – takes away the ability to come up with a strategy quickly enough to not get caught up in the ramp of intensity of ordinary emotions.
Inflammation tends to disrupt the “off-switch” for ordinary and amygdaloid intense emotion.
Lately I’ve been favoring amino acids – glutamate for energy, motivation, appetite to get up, GI tract healing; and 5-HTP to get to the 5-HTP4 receptor that seems to be pivotal for both anxiety, depression and mood intensity.
We had been having success with clemastine 1.34 mg po qhs for restoring white matter fiber-bundle myelination (which had been available over the counter in the US). But reading Robert Naviaux on “Metabolic features of chronic fatigue syndrome”, PNAS 2016, I am wondering if you have some thought about how to support myelination considering Naviaux found decreased activity of the sphyngomyelin and phosphomyelin pathways that seem to be necessary for demyelination.
Thanks for you website and helping people the way you do.
Inder Singh Virdi BA (Hons) mBANT · August 11, 2021 at 2:35 pm
Hi Daniel, I hope you’re well and my apologies for the delay in response. What a fascinating question: I think it largely depends on the etiological process driving ‘demyelination’. If there is autoimmunity involved one must identify and remove the triggers. I’ve found addressing a low-grade viral infection such as HHV-6 or EBV has helped my clients tremendously. I dose B12 has also been extremely effective. I really like B12-2000 from Biotics research. Hope this helps. Inder
Stephanie · November 3, 2021 at 3:31 am
What do you use to address clients ebv?
Silvi · December 15, 2021 at 2:26 pm
hello, looking for information on the gupta program I discovered your site. I saw this post is from October 2020, how are you feeling now? have you had any improvements with the program, are you healed?
Do you know anyone who has been healed using it?
I am going to buy it but I would like to know if it really works. I have spent hundreds of euros on supplements, therapies and doctors, I also want to try the Gupta program but I would like to read some positive results that are not sponsored by the Gupta site
Thank You very much
Inder Singh Virdi BA (Hons) mBANT · December 22, 2021 at 1:37 pm
Hi Silvi,
Yes, I am much better thank you. I am now running my clinic and living a fairly ‘normal’ life. Like you, I’ve spent thousands on many trendy supplements and programmes. I will say using the Gupta programme together with a targeted nutritional therapy or functional medicine programme will help address all the factors contributing to chronic fatigue. I still use parts of the programme when I’m especially stressed. Hope this answers your question.
damana game · July 28, 2025 at 3:04 pm
Thank you for sharing your experience with the Gupta Retraining Program! It’s inspiring to hear how it has made a difference for you in managing Chronic Fatigue Syndrome. I’ve been considering trying it myself, and your insights give me hope. I’d love to know more about any specific techniques that helped you the most during the program!
Inder Singh Virdi BA (Hons) MSc · November 10, 2025 at 2:42 pm
Hi Damana, for me it was a combination between the alternate nostril breathing, meditation and 7-step process. It’s overwhelming at first but it’s really about finding what works and resonates for you.
gringoxp · October 17, 2025 at 12:40 pm
Thank you for sharing your journey with the Gupta Retraining Program. It’s inspiring to see how you’ve navigated your challenges with Chronic Fatigue Syndrome. Your insights on the program’s approach and its impact on your life are invaluable. I’m curious, did you experience any initial doubts about the techniques, and how did you overcome them? Looking forward to hearing more about your progress!
Inder Singh Virdi BA (Hons) MSc · November 10, 2025 at 2:43 pm
I absolutely experienced doubts when I started it. I may have mentioned in the article, I found Ashok and voice quite annoying and I didn’t want it to work so I could get my money back. This was the most convincing evidence for me, that despite my dislike of him, I followed the steps and the rest is history.